Modulating gut microbiota in metabolism disorders and alcoholic hepatitis
Literature selection
By Pr Markku Voutilainen
Turku University Faculty of Medicine; Turku University Hospital, Department of Gastroenterology, Turku, Finland
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
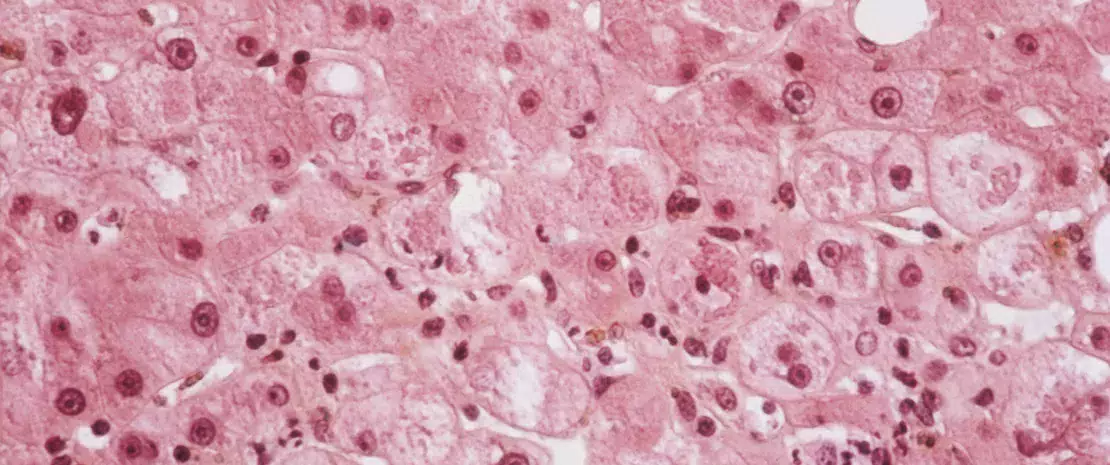
Alcoholic hepatitis. Light micrograph of a section through a liver affected by hepatitis (inflammation of the liver) caused by excessive alcohol intake.
About this article
Author
Gut microbiome fermentation determines the efficacy of exercise for diabetes prevention
The impact of exercise on gut microbiota was examined in prediabetic men. Exercise responders had a decrease in fasting insulin and insulin resistance (HOMA-IR), whereas in non-responders they remained unchanged or even deteriorated. Exercise caused increased abundance of Firmicutes, Bacteroides, and Proteobacteria. Alterations of the gut microbiota correlated with the reduction of HOMA-IR. DNA synthesis, amino acid (AA) metabolism, and short chain fatty acid (SCFA) synthesis enhanced in responders. In non-responders, AA fermentation was shifted to production of colonic gases and detrimental compounds, which associate with increased insulin resistance. Increased serum short chain fatty acids, but decreased branched chain amino (BCAA) and aromatic amino acids were detected only in responders. SCFAs have a beneficial role in energy and glucose metabolism, whereas increased BCAAs associate with insulin resistance.
In conclusion, exercise responders’ gut microbiome had enhanced capacity to produce short chain fatty acids but increased breakdown of BCAAs, whereas the microbiome of non-responders produced metabolically detrimental compounds.
Bacteriophage targeting of gut bacterium attenuates alcoholic liver disease
Alcoholic hepatitis (AH) patients have increased fecal Enterococcus faecalis (EF), 80% of AH patients are positive for EF. Germ-free mice on ethanol diet were colonized with cytolysin-positive (CL) EF feces of AH patients. Those infected with CL + feces developed a more severe ethanol-induced liver damage. Mice having overgrowth of intestinal enterococci and on ethanol diet were given bacteriophages lysing CL + EF. They developed less severe liver damage. Thus phage therapy may attenuate ethanol-related liver disease caused by CL + EF and improve prognosis in severe AH









