Skin microbiota : which role in atopic dermatitis and acne?
Literature selection
By Pr Markku Voutilainen
Turku University Faculty of Medicine; Turku University Hospital, Department of Gastroenterology, Turku, Finland
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
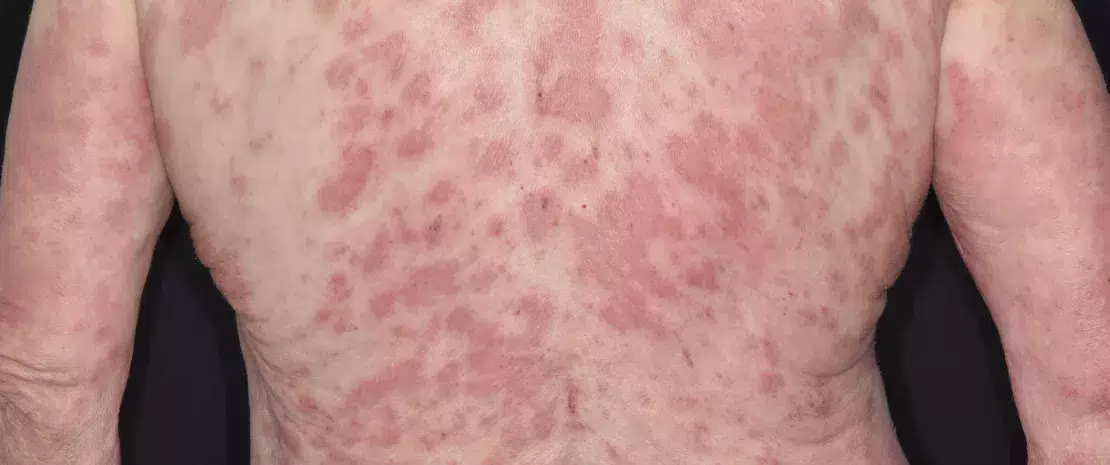
Atopic dermatitis on the upper body of an 83 year old male patient. Atopic dermatitis, also called atopic eczema, is an inflammatory skin reaction that occurs without any obvious external cause.
About this article
Author
Microbe-host interplay in atopic dermatitis and psoriasis
The authors compared atopic dermatitis (AD) and psoriasis (PSO) microbiota with that of healthy volunteers. The authors detected 26 and 24 microbes typical for AD and PSO, respectively. The most discriminative taxa for AD were genus Staphylococcus, and most discriminating microbes for PSO were Corynebacterium simulans, Neisseriaceae g. spp., C. kroppenstedtii, Lactobacillus spp. and L. iners.
AD is characterized by S. aureus abundance. In PSO, many different bacteria such as Corynebacterium may be involved. The depletion of Lactobacillus is typical for both diseases. In AD, loss of strictly anaerobic bacteria is typical with diminished production of lactic and short chain fatty acids leading to increased skin pH. Microbe-host interactions are important both in skin homeostasis and disease pathogenesis.
Staphylococcus epidermidis: a potential new player in the physiopathology of acne?
The interplay between skin and cutaneous microbiota is essential to differentiate between commensal and pathogenic bacteria. During puberty, over-colonization of skin pilosebaceous units (PU) by Cutibacterium acnes (CUA) may cause acne. Some strains of S. epidermidis modulate host innate immune reactions, and some isolates have antimicrobial activity against CUA. Conversely, some CUA strains have antimicrobial activity against S. epidermidis which may also control CUA via succinic acid. The use of topical antibiotics may result in the development of antibiotic-resistant strains of CUA and S. epidermidis. Eliminating only CUA may lead to proliferation of S. aureus and S. epidermidis increasing the risk of infections. Lactobacillus may be efficient in acne and other inflammatory skin diseases. The authors suggest that regular oral or topical supplementation of skin microbiota could be treatment option in acne.








