Skin Microbiota #11
By Prof. Markku Voutilainen
Turku University Faculty of Medicine; Turku University Hospital, Department of Gastroenterology, Turku, Finland
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
About this article
Author
THE ROLE OF SKIN MICROBIOTA IN ITCH
Kim HS, Yosipovitch G. The Skin Microbiota and Itch: Is There a Link? J Clin Med 2020 ; 9 : 1190.
The authors discuss the role of skin microbiota in the pathogenesis of itch. Itch sensation is mediated via epidermal nerve fibres (pruriceptors) driving by chemical mediators that originate from a complex interaction between keratinocytes (KC), inflammatory cells, nerve endings and the skin microbiota, relaying itch signals to the brain. Skin dysbiosis is characterized by production of proteases, pathogen-associated molecular patterns, and toxins, leading to skin barrier damage. Mast cell degranulation induced by delta-toxin prompt inflammation and itching. Skin microbiota and brain communicate via neurochemicals (acetylcholine, histamine, catecholamines, corticotropin) originate from skin microbiota. Stress intensifies itch via the skin-brain axis, where the amygdala seems to modulate itching sensation via microbial signals. Chronic stress increases cortisol production, directly activates skin bacteria by increasing the virulence of skin pathogens, leading to a weakening of the skin barrier and to an aggravation of the itch sensation. The authors conclude that cosmetics/transdermal drugs that modulate skin microbiota might have the potential to ameliorate itch.
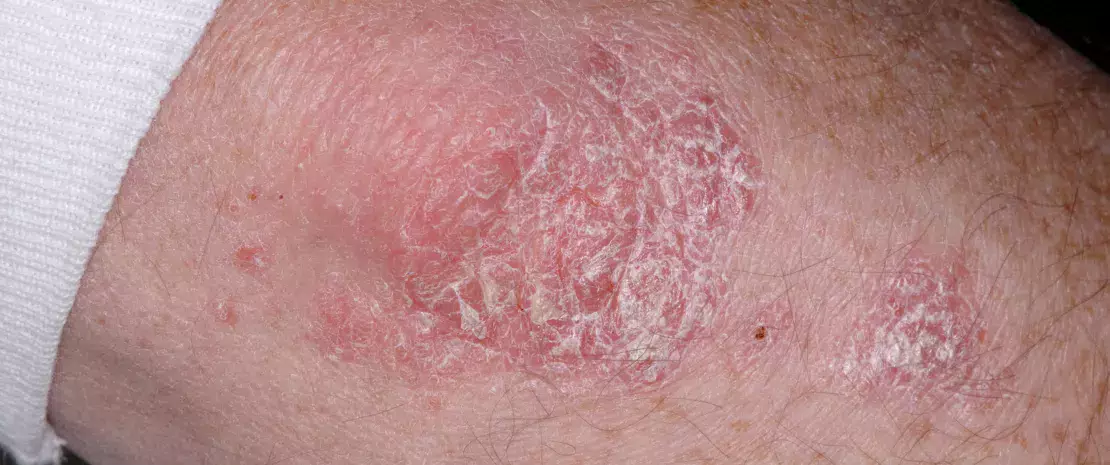
SKIN MICROBIOTA IN PSORIASIS
The authors examined the microbiota in psoriatic lesions and unaffected skin in psoriasis vulgaris (PS) patients and healthy controls by quantitative PCR and 16S rRNA sequencing. Higher bacterial load and lower diversity was observed in PS lesions than patients unaffected and controls’ skin. Cutibacterium (Cu) was reduced in lesions, whereas Corynebacterium (Cr) was increased. Compared with patients’ unaffected skin, Cr/Cu + Cr ratio was higher in the lesions. These findings indicate that PS was the major cause for the imbalance between Cu and Cr between lesions and unaffected skin or controls. Cr load correlated with the severity of PS lesions, whereas Cu load showed correlation with the abnormity of skin capacitance. The present study suggests that skin microbiota might play a significant role in the pathogenesis of PS.








