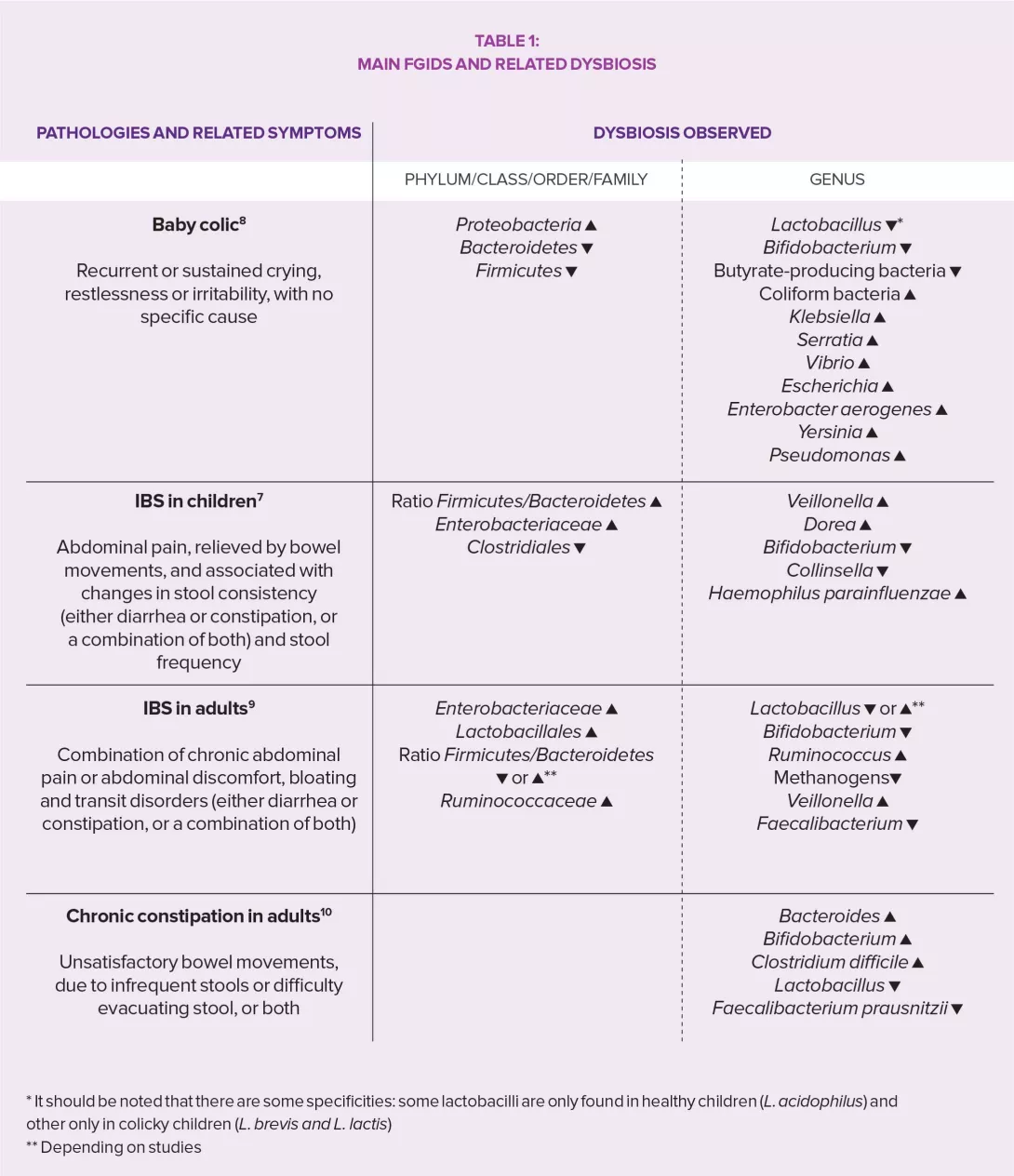
In newborns
Functional gastrointestinal disorders are liable to manifest themselves from the first moments of life. The predominating pathologies vary according to age, but are accompanied by extensive involvement of the intestinal microbiota.
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections

About this article
The main FGID in infants is colic. This disorder, whose pathophysiology is poorly understood, could originate in the microbiota and is thought to warrant new therapeutic approaches, as the efficacy of standard treatments has proven variable from one individual to another.
A DISEASE WITH IMPRECISE BOUNDARIES
Baby colic has an estimated prevalence of 5% to 28% depending on the study, and is a benign syndrome characterized by recurring bouts of crying, often accompanied by physical symptoms: clenched fists, straightened legs, facial redness. Appearing classically at around two weeks old, it reaches peak severity between 5 to 8 weeks and resolves spontaneously at around the age of 4 months. Its pathogenesis is still unclear, and diagnosis is currently based on Rome IV criteria. Organic causes are thought to represent only a small proportion of causes involved (5%). Additional factors such as an allergy to cow’s milk protein, family tensions and anxiety, etc. are likely to play a part.
CURRENT TREATMENTS
The diversity of causes makes patient care complex and encourages the diversification of treatment options, rendering treatment non-specific. What are the main current approaches? Drugs (mucosal protective agents, antispasmodics…), diet (modified diets, especially formulas based on casein hydrolysate, whey or soy milk…), behavioral techniques (chiropractic, reduced stimulation of the child…) and some probiotics.
INNOVATIVE ETIOLOGICAL HYPOTHESES INVOLVING THE MICROBIOTA
An international team has proposed three etiological hypotheses which could lead to new therapeutic approaches: first of all, immaturity of the enterohepatic circulation and of the action of bile acids leading to malabsorption of fats and other nutrients, as well as possible side effects on the intestinal microbiota.8 Secondly, intestinal dysbiosis, triggering an increase in nutrient fermentation and reduced levels of dehydroxylated bile acids in the colon. Finally, immaturity of the enteric nervous system resulting in abnormal sensorimotor function in the intestines and colon. The future characterization of these three mechanisms, which display numerous potential interactions, could lead to a more specific diagnosis and personalized management based on targeted biomarkers.8