Modulating the skin microbiota with oral solutions
The existence of a gut-skin axis suggests the possibility of influencing the skin microbiota by modulating the gut microbiota. Pre- and probiotic oral solutions are therefore an option.
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
About this article
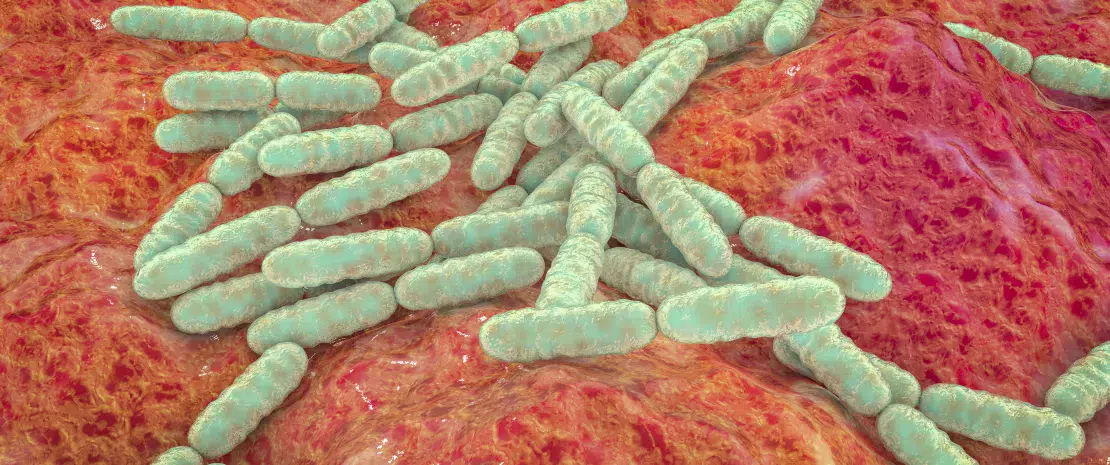
In numerous murine models, a Lactobacillus-enriched diet reduces skin sensitivity, rash, inflammation, dermatitis, etc., and improves skin phenotype (increased dermal thickness, enhanced folliculogenesis and increased sebocyte production).23 These beneficial probiotic effects have been confirmed by several interventional studies in humans involving lactobacilli and/or bifidobacteria.23 Managing skin diseases by modulating the gut microbiota will most likely involve probiotics (beneficial live bacteria), prebiotics (bacterial substrates) and symbiotics (combinations of pro- and prebiotics).23
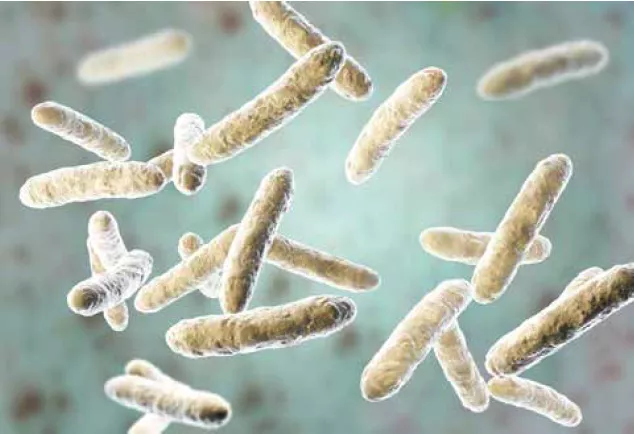
In mice, a Lactobacillus-enriched diet reduces skin sensitivity and improves skin phenotype.
A lack of adverse effects makes oral probiotics of even greater interest for the management of skin diseases.14
For example, in atopic dermatitis, daily consumption of probiotics (Bifidobacterium) and prebiotics (galacto-oligosaccharides) improves skin hydration in healthy adult women.14 To take another example, oral Lactobacillus supplementation reduces skin sensitivity and strengthens the skin’s barrier function in adults29 and children30. Several clinical trials have shown probiotics to have a positive effect when taken alone or in a cocktail (lactobacilli, bifidobacteria and/or S. thermophilus), with a reduction in lesions and severity in the case of acne.12,23 The positive effects of oral probiotics may be due to their ability to reduce systemic oxidative stress, regulate cytokines and reduce inflammatory markers.9 In the case of psoriasis, there are still few clinical data, but two studies in humans show beneficial effects: a reduction in inflammation markers with B. infantis; a reduction in the severity and appearance of lesions with B. longum, B. lactis and L. rhamnosus alongside a topical corticosteroid treatment.13 There were similar results for seborrheic dermatitis, with inflammation and symptoms relieved by oral L. paracasei.12 Some probiotics may even protect against skin cancer.16 However, clinical trials are still required to identify the most effective formulation of probiotic strains, the optimal duration of supplementation and the patients most likely to benefit.14







