Factors affecting the skin microbiota
The skin microbiota of healthy individuals appears to be relatively stable over periods of a few months or years.3,4 However, its composition is still influenced by the host and its environment.
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
Staphylococcus epidermidis
About this article
HOST-RELATED EFFECTS
The composition of the skin microbiota is strongly influenced by the host, specifically by their age, sex, genes, immune status, concomitant health conditions (dermatological or otherwise), the skin area in question, interactions between microorganisms, diet and stress levels.2
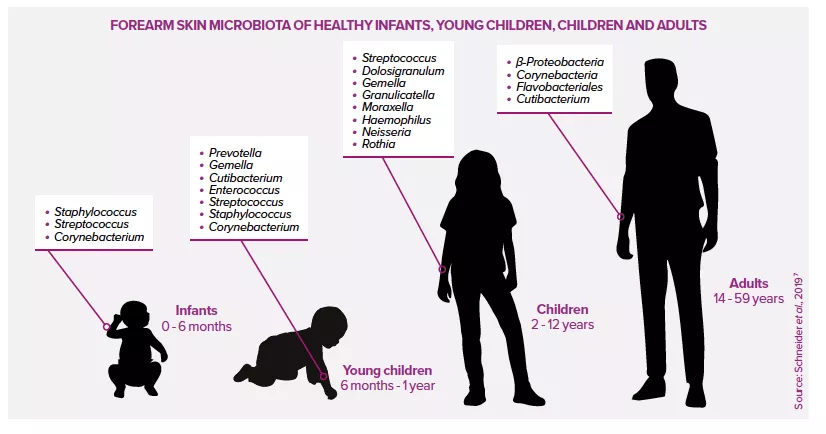
The initial colonization of a newborn baby’s skin depends on the mode of delivery4,7: children born vaginally acquire vaginal bacteria (Lactobacillus, C. albicans), while those born by caesarean section acquire skin microbes (Staphylococcus, Streptococcus). Within a few hours of birth, sebum secretion increases sharply. This continues for several days before decreasing.2 The immature immune system facilitates colonization due to the lack of any inflammatory response.4
At puberty, the skin microbiota undergoes a profound restructuring due to hormonal changes that stimulate sebaceous secretions. It contains more lipophilic organisms (Cutibacterium, Malassezia), whereas previously it had been dominated by Firmicutes, Bacteroidetes and Proteobacteria, with a diverse fungal community.4
ENVIRONMENTAL EFFECTS
Many external factors also influence the composition of the skin microbiota2, including lifestyle, domestic and personal hygiene, cohabitation, geographical location, sunlight, occupation (and work clothing), etc. For example, contact with other humans, but also with pets and objects (telephone, computer keyboard, classroom objects, etc.), modifies the skin microbiota and explains the similarities observed between the microbiota of members of the same household or group.3
Moreover, the conditions in a given environment affect the different areas of the skin to different degrees. For example, some skin areas (e.g. hand) have more physical contact, others are less exposed to ultraviolet light, etc.3,4 Despite this, the skin microbiota remains relatively stable in adulthood, suggesting reciprocal beneficial interactions between microorganisms and host.6







