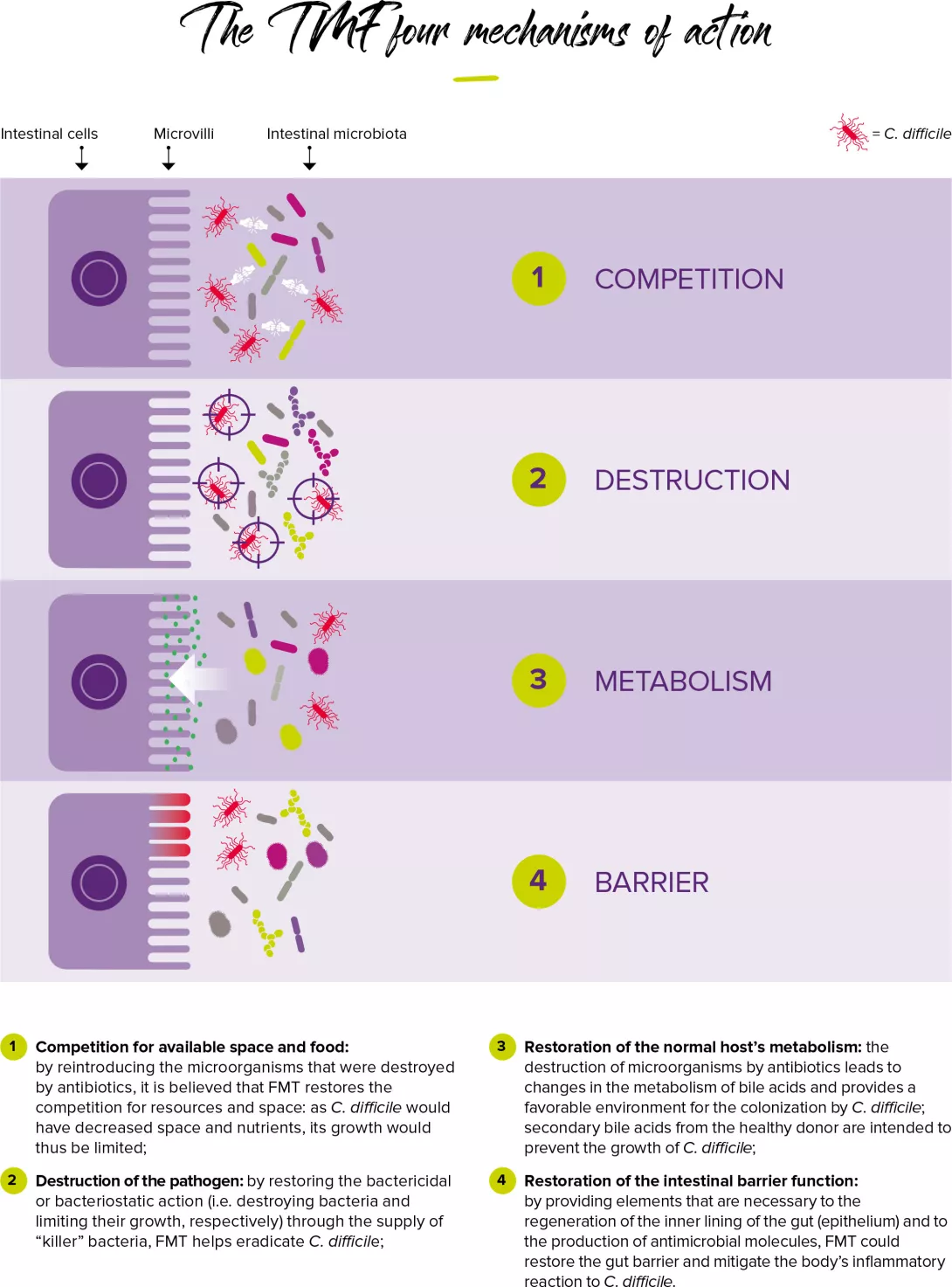
The mechanism of FMT: transplanting to restore the balance
Although the media only recently became interested in this topic, fecal microbiota transplant is actually a very old medical practice. Its history goes all the way back to 4th-century China. It was then called “yellow soup” and was used to treat diarrhea and food poisoning. But the first experiment with a fecal enema was only conducted in 1958. In 2013, 45 years later, the results of the first clinical trial on FMT were published, demonstrating that it is superior to antibiotics in the treatment of recurrent Clostridium difficile infections1, a bacterium which is responsible for 20 to 30% of antibiotic-associated diarrhea that can sometimes be severe. It was the start of the craze towards FMT, first from researchers and later from the general public.