Targeting the gut microbiota to optimize vaccine efficacy?
by Dr Genelle Healey
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
About this article
Author
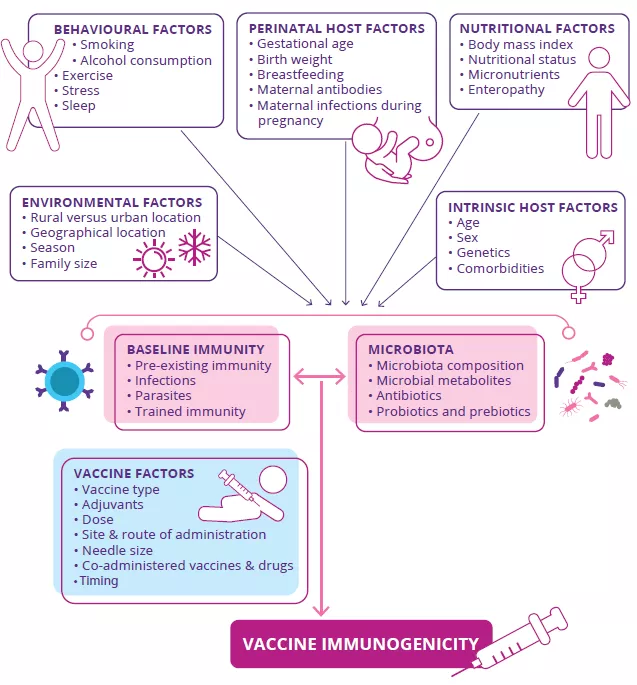
Since the COVID-19 pandemic started, the need for a robust and long-lasting immunity induced by vaccines has never been more apparent.20 However, vaccine- induced immune responses are highly variable between individuals and many factors have been suggested that may alter vaccine immunogenicity and efficacy (Fig 8).21Therefore, gaining a better understanding of the factors driving variations in vaccine efficacy is critically important.
Vaccine-induced immune responses are highly variable between individuals and many factors have been suggested that may alter vaccine immunogenicity and efficacy. One factor known to control vaccine efficacy can be the gut microbiota.20
One factor known to control vaccine efficacy is the gut microbiota.21 Interestingly, certain gut microbiota profiles (i.e. higher abundance of Actinobacteria, Clostridium cluster XI and Proteobacteria) are associated with greater vaccine responses against other viral infections such as HIV and rotavirus.22-26 Additionally, a recent study reported that antibiotic-induced intestinal microbiota dysbiosis led to impaired vaccine responses against influenza, such as a reduced antibody-based neutralization of the virus, as well as lower concentrations of antibodies produced in responses to vaccination.27 This and other similar studies provide evidence of the important role that the gut microbiota plays in vaccine efficacy.23,28
FIGURE 8: Factors suggested to alter vaccine immunogenicity and/or efficacy, including intrinsic host factors, behavioural, environmental, nutritional and perinatal factors.
Most of these factors have also been shown to influence the composition of the gut microbiota and baseline immunity. Vaccine immunogenicity is also dependent on vaccine intrinsic factors.
Adapted for Lynn DJ et al, 202120
To date no studies have investigated what impact the gut microbiota may have on SARS-CoV-2 vaccine efficacy, but it seems likely that individuals with gut microbiota dysbiosis may be at increased risk of developing relatively poor vaccine responses. Thus, future research which examines whether specific gut microbiota signatures affect SARS-CoV-2 vaccine efficacy will be critically important.