Gut-lung axis in viral respiratory infections
By Dr Genelle Healey
Lay public section
Find here your dedicated section
Sources
This article is based on scientific information
Sections
About this article
Author
Interestingly, microbiota at both tissue sites appear to be perturbed during respiratory infections, reinforcing the theory that all mucosal sites are interconnected and that the gut-lung axis is bidirectional.1
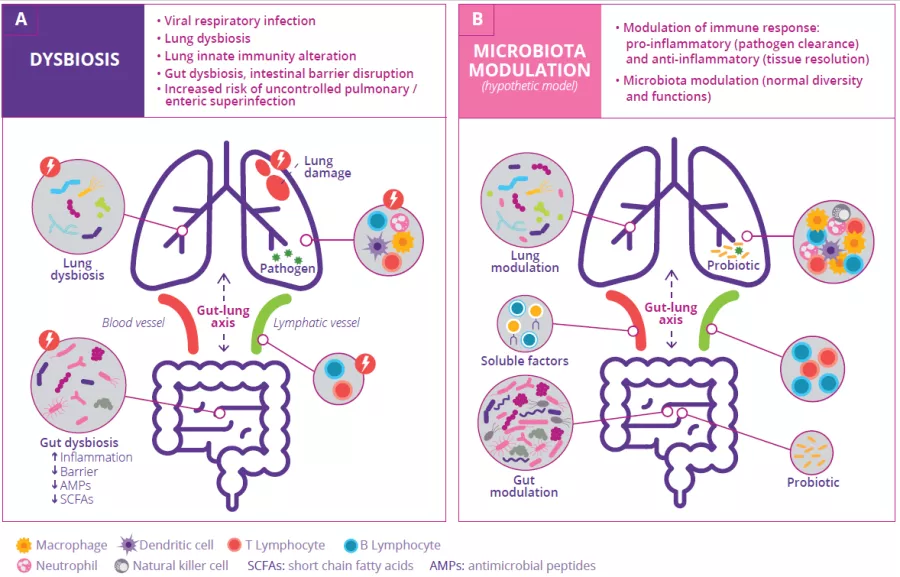
Gut bacteria, their fragments, as well as SCFAs may translocate across the intestinal barrier and travel along the mesenteric lymphatic system to reach the systemic circulation and modulate immune cells in the lung.11 During Influenza respiratory infections, lung microbiota and immune functions are altered, and a gut microbiota dysbiosis is also observed which may explain the commonly associated gastroenteritis-like symptoms (Fig 7A).10
FIGURE 7: Gut-lung axis during viral respiratory infection (A) and model of microbiota modulation using probiotics (B).
Adapted from Dumas A et al, 20182
Probiotics may be helpful to recover a healthy status (microbiota homeostasis, infection control, modulation of immune responses) via gut microbiota metabolites (SCFAs…) or host-derived products.
There are likely several causes of this gut dysbiosis including loss of appetite (leading to reduced food and calorie intake), as well as inflammatory cytokine release. This may have local consequences: intestinal inflammation, disruption of gut barrier, decreased production of antimicrobial peptides (AMPs), a drop in SCFAs, potentially leading to secondary enteric infections.10
Gut barrier alteration promotes bacterial translocation as well as endotoxin release into the blood, leading to systemic inflammation, lung damage aggravation and increased risk of secondary bacterial infections.10 The reduced SCFA production by the gut microbiota also contributes to the reduced antibacterial immunity seen in the lungs.10 This highlights the vital role that the gut microbiota plays in the lung’s defenses against respiratory infections.
Modulation of the gut microbiota using strategies such as probiotics may help reduce susceptibility to respiratory infections via the gut-lung axis, or they may be helpful in recovering from infection and reaching a healthy status (Fig 7B). Several studies in mice have shown that specific probiotics administered prior to influenza infection led to the reduced accumulation of immune cells in the infected lungs. These probiotics also enhanced viral clearance, improved overall health and reduced alterations in the gut microbiota.12,13
Recommended by our community

"Well, I'm one among people with lung problem (infection)
I get this so important." -@Ahishakiyejanv2 (From Biocodex Microbiota Institute on X)