Antimicrobial resistance: a universal threat, an international response
It could ultimately undermine a century of medical progress1. The ticking health time bomb of antimicrobial resistance is in sights of the WHO, which has organised the annual World AMR Awareness Week (18–24 November) since 2015. The Microbiota Institute plays an active role in this initiative, producing and sharing exclusive content throughout November on the impact of antimicrobials on the gut microbiota. We take a quick look at what's happening.
- Learn all about microbiota
- Microbiota and related conditions
- Act on your microbiota
- Publications
- About the Institute
Healthcare professionals section
Find here your dedicated section
Sources
This article is based on scientific information

About this article
On the one hand, they are an extraordinary scientific discovery that saves millions of lives. On the other, their excessive and sometimes inappropriate use can lead to the emergence of multiple forms of resistance in microorganisms (including bacteria, viruses, parasites and fungi). As a result, although they were designed to heal, antimicrobials are becoming less and less effective and, ultimately, if no action is taken, there is a risk that they will no longer be able to protect us from infections.
Antimicrobial resistance would become responsible for almost 700,000 annual deaths worldwide2. If nothing changes, infectious diseases could become one of the leading causes of mortality worldwide by 2050, causing up to 10 million deaths2.
10 million Antimicrobial resistance would become responsible for almost 10 million deaths worldwide by 2050
The WHO is spearheading the international response to this scourge. Since 2015, it has organised World AMR Awareness Week, held on 18–24 November, which aims to increase awareness of this global phenomenon and encourage the general public, healthcare professionals and decision-makers to use antibiotics carefully, to prevent the further emergence of antimicrobial resistance.

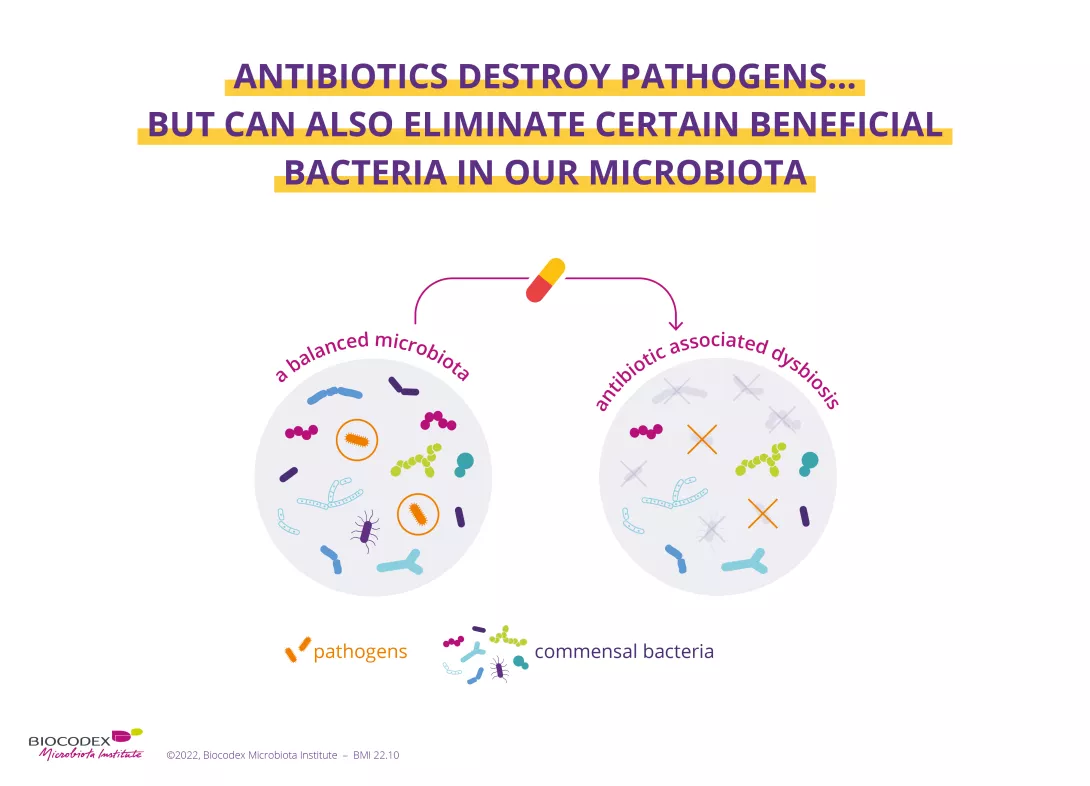
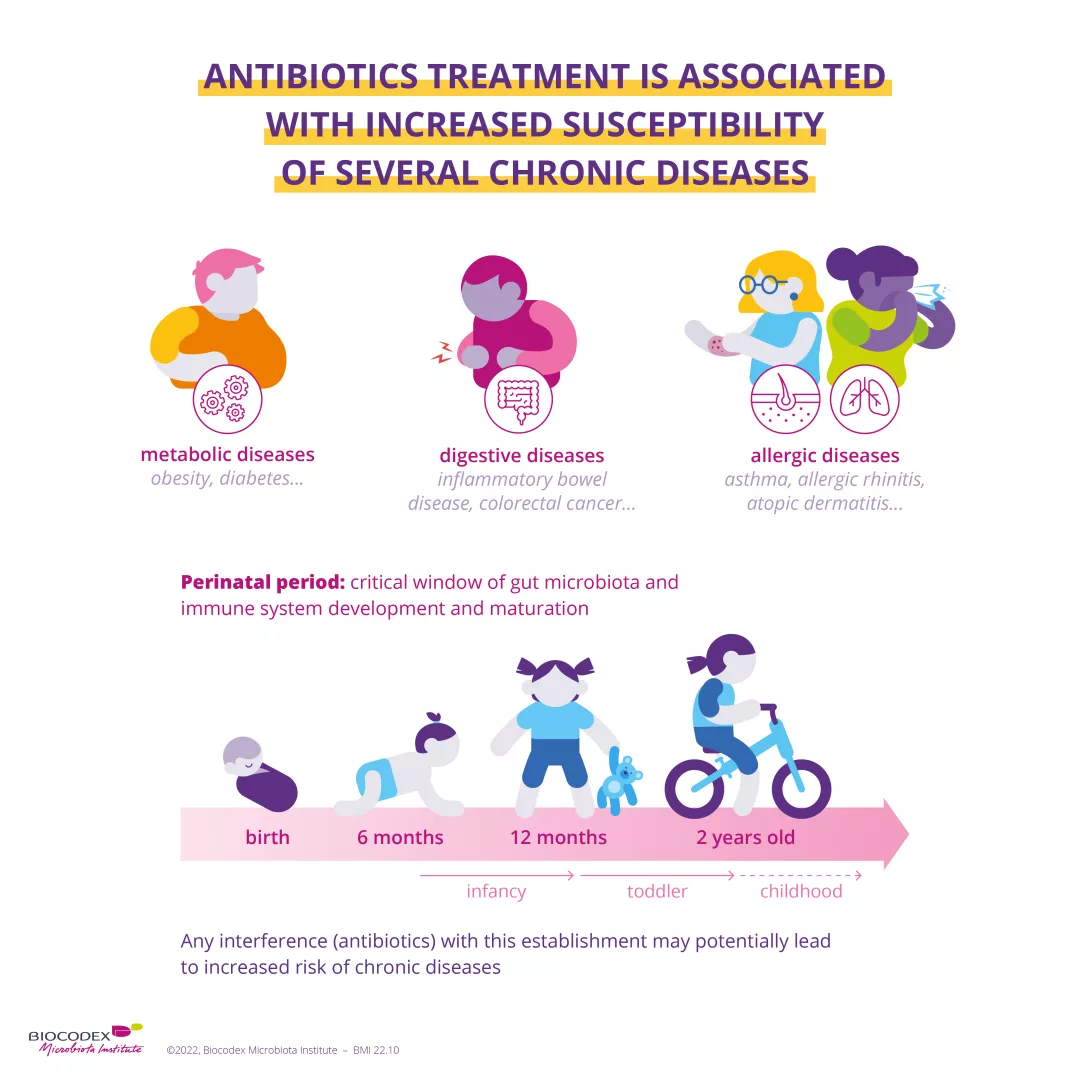
As a major centre of expertise on the microbiota, the Microbiota Institute has been an active partner for the event since 2020. Throughout November, the Institute will be sharing articles and news, as well as expert videos, to help you understand the mid- and long-term effects of antibiotics on the human microbiota. To cite just one example, despite their well-known efficacy against bacteria (and lack of efficacy against viral infection3), antibiotics disrupt the balance of our gut microbiota. This imbalance, more commonly known as (sidenote: Dysbiosis Generally defined as an alteration in the composition and function of the microbiota caused by a combination of environmental and individual-specific factors. Levy M, Kolodziejczyk AA, Thaiss CA, et al. Dysbiosis and the immune system. Nat Rev Immunol. 2017;17(4):219-232. ) , is associated with several well-known problems, such as antibiotic-associated diarrhea. But there's more! Taking antibiotics is also suspected to increase the risk of multiple chronic diseases (allergies, asthma, obesity, chronic inflammatory bowel disease, etc.), particularly if they are prescribed in early childhood.
So can we do anything about it? Yes! Firstly, by ensuring that antibiotics are used sensibly and appropriately. Do not take these medications without a prescription from a healthcare professional. Stick to the specified dose, administration frequency and duration of treatment and do not share your antibiotics with anyone else4. And remember, as the French health slogan states:
Antibiotics: handle with care© !
If you are interested in the effects of antibiotics on your health and your microbiota, or if you want to know more about the World AMR Awareness Week (WAAW), we recommend that you go to this other dedicated page:
Antibiotics: what impact on the microbiota and on our health?
Each year, since 2015, the WHO organizes the World AMR Awareness Week (WAAW), which aims to increase awareness of global antimicrobial resistance.
Antimicrobial resistance occurs when bacteria, viruses, parasites and fungi change over time and no longer respond to medicines. As a result of drug resistance, antibiotics and other antimicrobial medicines become ineffective and infections become increasingly difficult or impossible to treat, increasing the risk of disease spread, severe illness and death.
Held on 18-24 November, this campaign encourages the general public, healthcare professionals and decision-makers to use antibiotics, antivirals, antifungals and antiparasitics carefully, to prevent the further emergence of antimicrobial resistance.
2. Tackling drug-resistant infections globally: final report and recommendations; May 2016.
3. Improving Antibiotic Use. Material Developed by CDC Using CDC materials does not imply endorsement or recommendation by CDC, ATSDR, HHS or the United States Government
4. Taking your Antibiotics. Material Developed by CDC Using CDC materials does not imply endorsement or recommendation by CDC, ATSDR, HHS or the United States Government
Recommended by our community

"Thanks for sharing!" -Gigi Snook (From My health, my microbiota)
"Nice 👍🏾" -Lucy Ofreneo (From My health, my microbiota)
"Interesting!" - Rémi Fresnel (From Biocodex Microbiota Institute on LinkedIn)













