The gut microbiota
Gut microbiota: why is it that important for your health?
We have trillions1 of bacteria that populate our intestine with fascinating powers on the human body. Let’s understand how your intestinal microbiota works and why you should take care of it!
- Learn all about microbiota
- Microbiota and related conditions
- Act on your microbiota
- Publications
- About the Institute
Healthcare professionals section
Find here your dedicated section
Sources
This article is based on scientific information
Sections

About this article
Table of contents
Table of contents
What is exactly the human gut microbiota?
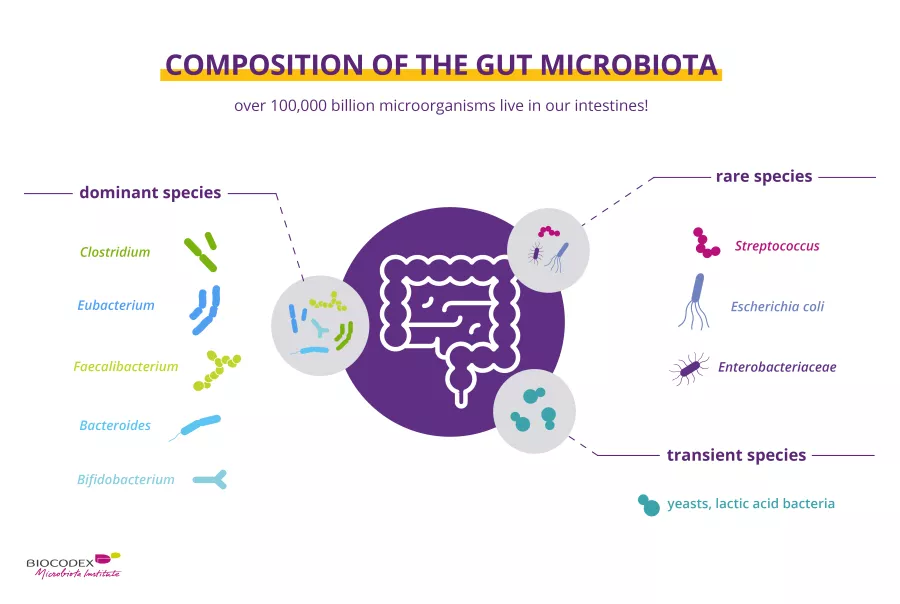
You probably have already heard about the “gut flora”, well, scientifically, it is called “the intestinal microbiota” or to put it more simply “the gut microbiota”. What is the definition of gut microbiota ? It consists of trillions1 of (sidenote: Microorganisms Living organisms that are too small to be seen with the naked eye. They include bacteria, viruses, fungi, archaea and protozoa, and are commonly referred to as “microbes”. What is microbiology? Microbiology Society. ) that populate your intestines like bacteria, viruses, fungi (including yeasts), and even parasites.
By the way, microbiota and microbiome are two words often used as one to the other but they have two different meanings while microbiota is used to talk about the microorganism and answer the question “who is there?” basically the “individuals”, the microbiome talks about their genome “what is inside of them”2 to answer the question “what are they doing” meaning their function.
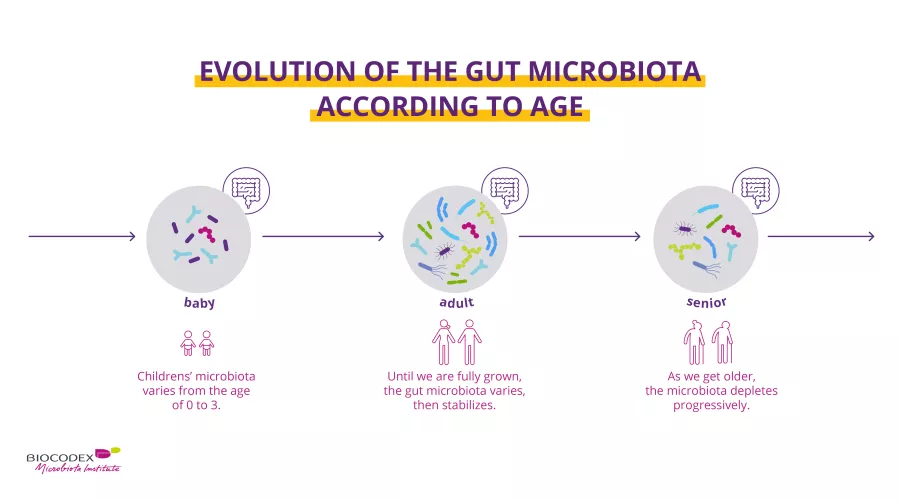
Each one of us has a unique microbiota, like a fingerprint.1 When you’re born, fecal and vaginal microorganisms transmitted by your mother during vaginal delivery, or environmental microorganisms for cesarean delivery,3 induce the start of your gut microbiota colonization4. It takes around three years for the gut microbiota to build up, diversify and stabilize.5 During adulthood,6 the composition is relatively stable until old age when it undergoes profound changes again to become slightly impoverished.7
100 000 100,000 billion “good” bacteria live in our gut
2nd the gut microbiota is often considered as the second brain
Why is gut microbiota important for your health?
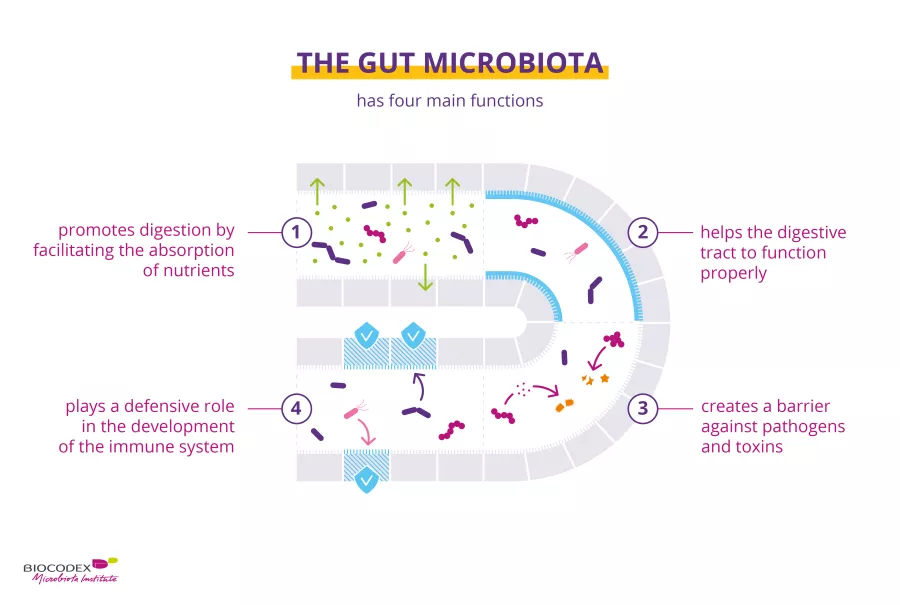
The gut microbiota can be considered a functional organ of the human body. Why should we take care of our microbiota ? It works closely with your intestines and have 4 important roles:
by helping with the absorption of nutrients (sugars, amino acids, vitamins…) by intestinal cells or with the fermentation of the small fraction of food. These fermentation processes produce gas and numerous metabolites, including short-chain fatty acids, a real “fuel” for the cells in your colon.8
by having an active role in the production of gastrointestinal mucus, the irrigation of intestinal cells, and the enzymatic activity of the mucosa.9
against pathogens and toxins.10 Furthermore, some bacteria release antimicrobial molecules against the (sidenote: Pathogens A pathogen is a microorganism that causes, or may cause, disease. Pirofski LA, Casadevall A. Q and A: What is a pathogen? A question that begs the point. BMC Biol. 2012 Jan 31;10:6. ) bacteria while others stimulate the production of mucus to protect intestinal cells from attacks and avoid harmful effects on your body.11
in developing the human immune system. Bacteria of the gut flora are involved in the maturation and activation of cells in the intestinal immune system, which protects you from attacks by pathogenic agents like bacteria and viruses. The intestine is the primary reservoir for immune cells in your body. For its part, the immune system influences the composition and diversity of microbiota.12
What affects your gut microbiota ?
The composition of the gut microbiota is characterized by its high diversity (number of different species present in an individual) and its abundance (total number of microorganisms present). When the composition is disrupted, the balance is broken, and a (sidenote: Dysbiosis Generally defined as an alteration in the composition and function of the microbiota caused by a combination of environmental and individual-specific factors. Levy M, Kolodziejczyk AA, Thaiss CA, et al. Dysbiosis and the immune system. Nat Rev Immunol. 2017;17(4):219-232. ) emerges,13 which can be associated with several diseases.
Numerous factors can have an impact on the diversity and composition of the gut microbiota. Among these factors, these are the following:
Factors linked to the individual themselves, such as:
- The age6
- Genetics13
- Certain illnesses and injuries13
Others factors are linked to the individual's environment:
- Medication use: antibiotics, anti-inflammatories, etc.8
- Infections (viral gastroenteritis…)13
- Lifestyle: unbalanced diet (high-fat diet for example), or changes in diet, stress, smoking, alcoohol excess, etc. 13
What are the diseases that could be linked to gut microbiota ?
Dysbiosis, cause or consequence of these diseases? The question has not yet been answered with certainty by scientific studies.
Let’s have a look to some diseases associated with intestinal dysbiosis:
-
Infantile colic 14 that affects 20 to 25% of infants between the age of 1 and 4 months
-
Antibiotics associated diarrhea, which happens between 5 and 35% of patients taking antibiotics15
-
Traveler’s diarrhea is an infection caused by contaminated food or contaminated. Postinfectious irritable bowel syndrome may occur in 3% to 17% of patients who had this infection16
-
Gastroenteritis generally benign and most often viral is responsible for over 200,000 deaths of children per year worldwide17
-
Obesity is a common, costly, and serious chronic disease that affected 13% of the world’s adult population (11% of men and 15% of women) in 201618
-
IBS is one of the most functional gastrointestinal disorders characterized by abdominal pain and alterations in the host’s bowel habits (constipation, diarrhea, or alternations). The prevalence varies substantially between countries19
-
Crohn’s disease is an inflammatory bowel disease, where inflammation can be localized at all stages of the digestive system, from the mouth to the anus. Recent studies provide evidence that the gut microbiota plays an important function in the etiopathogenesis of this disease20
-
Stomach cancer21 and colorectal cancer22 are two gastrointestinal cancers associated with gut microbiota dysbiosis
But the role of the human gut microbiota doesn’t stop at the gut: recent studies have identified that the gut microbiota may play a role beyond the gastrointestinal tract. In fact, gut microbiota has been associated with several extra-intestinal diseases: for example, acne23 , allergies24 , obesity,25 anxiety disorders,26 autism-spectrum disorders26…And that’s not all of it. It seems that gut microbiota can also be associated with neurodegenerative diseases like Alzheimer’s,27 Parkinson’s.28 In fact, there is bidirectional communication between the gut and the brain, named “gut- brain- axis”, and gut microbiota could influence these interactions. That is why your gut is sometimes called your second brain.
How to take care of your microbiota?
You know by now the central role of the gut microbiota in human health. So how should you take care of your own microbiota? How to improve your gut microbiota ? Many scientific studies raised the question of how to avoid any disruption in its composition and keep it as balanced as possible.29 The answer is not as simple as bring in good bacteria or yeast to fill or enrich the existing microbiota or replace the bad ones. In fact, the idea is to influence the microbiota to help it to function smoothly thereby improving host health.30
You have several ways of positively affecting the balance and the diversity of the gut microbiota :
-
Diet: the diversity and quality of what we eat contribute to the balance in our intestinal microbiota.31,32 On the other hand, a poorly balanced diet can affect the composition of our gut and lead to some conditions.33 It is important to know what type of food has a beneficial effect or a negative one to keep our gut in shape!34
-
Probiotics: Probiotics are live microorganisms that, when administered in adequate amounts, confer a health benefit on the host.35,36
-
Prebiotics: Prebiotics are specific non-digestible dietary fibers conferring a health benefit, they are selectively utilized by beneficial microorganisms in the host’s microbiota.37,38 Some foods are particularly rich in prebiotics, that’s why it is important to pay attention to our diet. When they are added to probiotics in some specific products, we call them symbiotics.39
-
Transplant: as for the organs, gut microbiota can be transferred to an individual in an attempt to restore equilibrium amongst the gut microbial ecosystem.32 Known as fecal microbiota transplant (FMT), this therapeutic approach is only validated to cure recurrent Clostridioides difficile–associated disease32 and is still under active research to evaluate its effect on other specific health conditions such as Crohn's disease, ulcerative colitis, irritable bowel syndrome, or metabolic disease32…
Oh! one more thing...
Now that you have read everything you need to know about the gut microbiota, you should also know that you have microorganisms all along the body: in your skin,40 your urinary tract,41 your vagina,42 your mouth,43 your ears,44 your lungs,45 and, as it does for the intestine, the microorganisms that live there play a tremendous role to keep them functioning and maintain you in health. To know more visit this page.
The Biocodex Microbiota Institute is dedicated to education about human Microbiota for General Public and Healthcare Professionals, it doesn't give any medical advice.
We recommend you to consult a healthcare professional to answer your questions and demands.
All the information in this article comes from scientific approved sources. Keep in mind this is not exhaustive. Here are all the studies from which we took all of that information
International Microbiota Observatory
BMI 21.10
11Sokol H. Microbiota and barrier effect. In: Marteau P, Dore J, eds. Gut Microbiota: A Full-Fledged Organ. Paris: John Libby Eurotext; 2017:65-71.
17 Stuempfig ND, Seroy J. Viral Gastroenteritis. In: StatPearls. Treasure Island (FL): StatPearls
18 WHO. Fact sheets on obesity and overweight June 2021
27 Qian XH, Song XX, Liu XL, et al. Inflammatory pathways in Alzheimer's disease mediated by gut microbiota. Ageing Res Rev. 2021 Mar 9;68:101317.