Women disorders
Candidiasis, bacterial vaginosis, cystitis... These infections can seriously affect the intimate health of women... and men too! The aim of this page is to provide you with essential information on the role of the microbiota in these pathologies. The knowledge shared here is designed to support women at every stage of their lives, from birth to menopause, and covers topics such as menstruation and pregnancy.

Breast cancer: efficacy of immunotherapy conditioned by the gut microbiota?
A recent study published in Cancer Research suggests that the gut microbiota affects responses to immunotherapy in HER2-positive breast cancer. How so? Via local and systemic modulation of the immune system.
The gut microbiota Can statins combat intestinal dysbiosis? What if manipulating the microbiota could improve the response to immunotherapy? What are the long-term effects of antibiotics on the gut microbiota?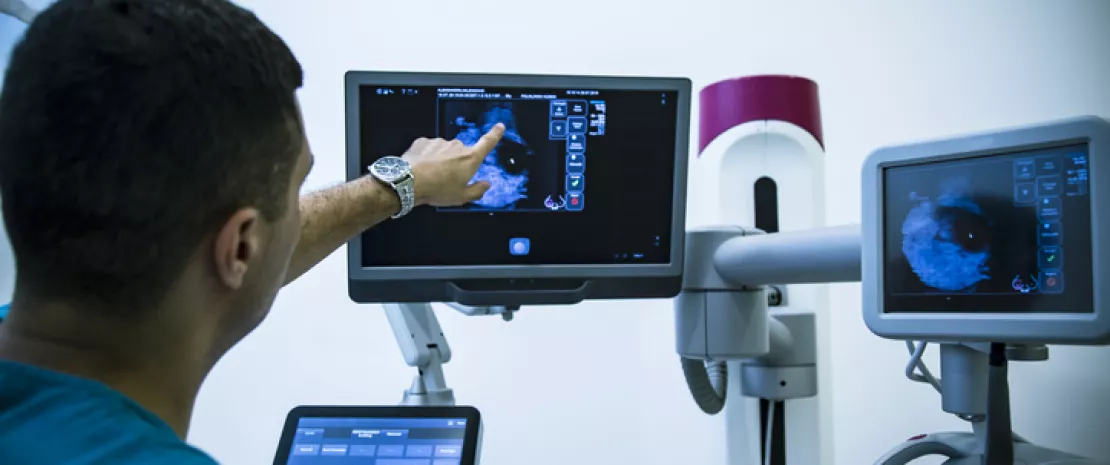
Is the gut microbiota a good indicator of longevity?
The older we get, the more unique our gut microbiota becomes. This uniqueness seems to predict healthy ageing and longer life expectancy among the elderly. All good reasons to pamper your microbiota!
The gut microbiota Diet
Sources:
Wilmanski T, Diener C, Rappaport N, et al. Gut microbiome pattern reflects healthy ageing and predicts survival in humans. Nat Metab. 2021 Feb;3(2):274-286.
The gut microbiota: a weighty factor in dieting
Tell me about your gut microbiota and I’ll tell you if you’ll lose weight: this is essentially the message of a Chinese research team which claims that our gut bacteria can predict our ability to lose weight during a diet.
The gut microbiota Metabolic syndrome Diet
 Post-diet weight gain: the microbiota’s anti-yo-yo effect
Post-diet weight gain: the microbiota’s anti-yo-yo effect
 Impact of bariatric surgery on gut microbiota
Impact of bariatric surgery on gut microbiota
Sources:
Jie Z, Yu X, Liu Y et al. The Baseline Gut Microbiota Directs Dieting-Induced Weight Loss Trajectories. Gastroenterology. 2021 Jan 20:S0016-5085(21)00096-2.
Melanoma: fecal microbiota transplant to overcome resistance to anti–PD-1?
A recent study published in Science shows that modulating the gut microbiota helps advanced melanoma patients respond to anti-PD-1 immunotherapy which their tumors had previously resisted. How? Thanks to fecal microbiota transplantation (FMT).
The gut microbiota What if manipulating the microbiota could improve the response to immunotherapy? Antibiotic exposure during first six years of life disrupts gut microbiota and impairs child growth Fewer antibiotics, less dysbiosis, less childhood asthma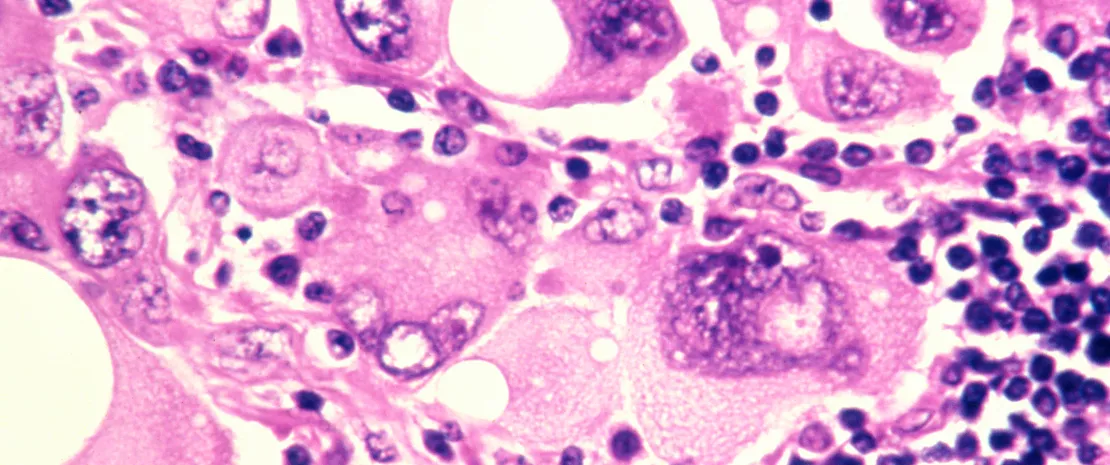
Can the lung microbiota reliably predict lung transplant rejection?
Predicting transplant rejection is every surgeon’s dream and every patient’s hope. According to a study published in The Lancet Respiratory Medicine, an increase in lung bacteria could predict chronic transplant rejection (chronic lung allograft dysfunction, or CLAD) in healthy adult lung transplant recipients.
The pulmonary microbiota Lung microbiota: a prognostic marker of COPD? The Janus face of Antibiotics: Life Savers and Microbiota Disruptors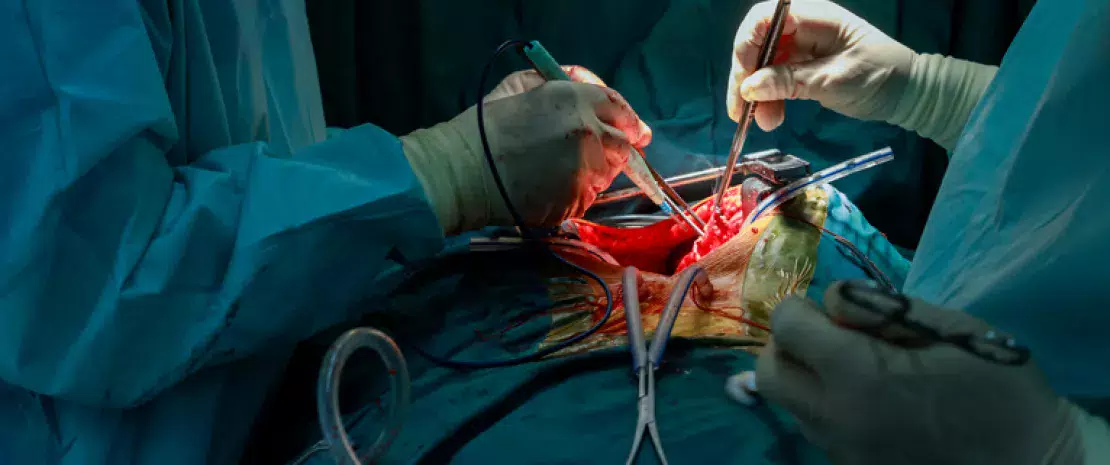
Dust microbiota from the city or the countryside? Atopic dermatitis has a preference!
With the lockdown, young children are spending a lot of time at home, surrounded by dust. Exposure to dust microbes may be a protective or risk factor for the development of atopic dermatitis, depending on whether a child lives in the city or the countryside.
The skin microbiota
Sources:
Mahdavinia M, Greenfield LR, Moore D, et al. House dust microbiota and atopic dermatitis; effect of urbanization [published online ahead of print, 2021 Feb 11]. Pediatr Allergy Immunol. 2021;10.1111/pai.13471. doi:10.1111/pai.13471





