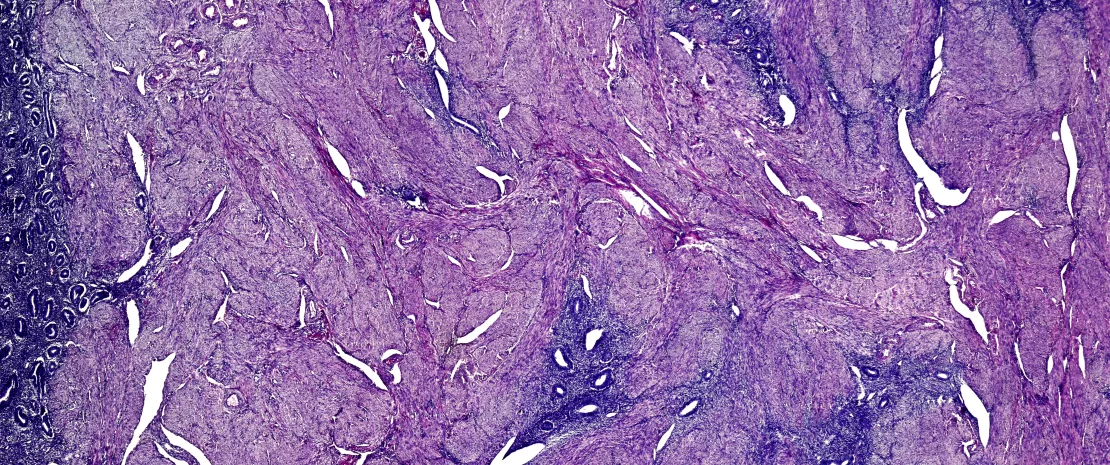
Endometriosis affects around 10% of women of childbearing age, with symptoms including dysmenorrhea, dysuria, pelvic pain, and reduced fertility or even infertility.
One diagnostic tool, laparoscopy, is invasive and delays treatment. Hence the hope of one day finding a non-invasive marker.
We may have to look no further, thanks to a study by Australian researchers who examined three microbiomes (oral, gut, and vaginal) to identify a bacterial signature of endometriosis.
Bacteria that signal disease...
Above all, the vaginal flora of the ENDO group was richer in Escherichia, Enterococcus, and Tepidimonas.
Their stools contained more Lactobacillus, but also more Phascolarctobacterium, a bacterium known to be more abundant in the peritoneal fluid of these patients, raising the hypothesis of a possible bacterial translocation from the gut to the peritoneum.
Furthermore, Fusobacterium was more abundant in the oral cavity: could this opportunistic pathogen, implicated in periodontal disease, explain the higher incidence of gum inflammation in women suffering from endometriosis?
... and its severity
Microbiota also appear to signal the severity of endometriosis:
- stools show a greater abundance of Actinomyces in cases of minimal/mild endometriosis (stages 1 and 2) and of Paraprevotellaceae in cases of moderate/severe endometriosis (stages 3 and 4);
- the oral microbiota is enriched with Cardiobacterium in cases of minimal/mild endometriosis and with Fusobacterium in cases of moderate/severe endometriosis;
- the vaginal flora contains more Blautia, Dorea, Collinsella, and Eubacterium in moderate/severe endometriosis.

 Why running could bring a smile to depressed teens... and their gut microbiota
Why running could bring a smile to depressed teens... and their gut microbiota
 Mental illness and the gut microbiota: the end of a riddle?
Mental illness and the gut microbiota: the end of a riddle?